The caregiver shortage is real. But many Canadian home-care agencies lose caregivers for reasons that have less to do with the labour market and more to do with what happens after someone applies.
Every owner knows the pattern. A promising applicant applies for a PSW job, then does not answer the phone. A caregiver accepts an interview, then disappears. A new hire completes some paperwork, but training drags. A first shift is offered, but the care plan is unclear, the travel time is awkward or the client is a poor fit. A caregiver who looked strong on Monday has moved on by Friday.
So the agency buys more job ads, posts again for “caregiver jobs near me”, “PSW jobs Ontario” or “home support worker jobs Canada”, asks staff for referrals and spends more time screening strangers. That may bring more applicants into the funnel. It does not fix the leak.
For Canadian senior-care agencies, the question is not only how to recruit caregivers. It is why so many are lost between the application, the interview, the first shift and the first month.
How should agency owners treat caregiver loss
Home-care agencies should stop treating caregiver loss as only a recruitment problem. The larger issue is the operating system behind recruitment: response speed, screening, structured interviews, background checks, document management, credential tracking, training, caregiver communication, first-shift preparation and early retention.
The labour market will not get easier soon. Canada’s occupational projection system projects 26,200 job openings for home support workers, caregivers and related occupations from 2024 to 2033, against 24,600 projected job seekers. Job Bank also describes the occupation as facing a strong risk of labour shortage and reports that almost half the workforce was aged 50 or older in 2023.
ConsidraCare’s platform is built around that operating problem. It includes an applicant tracking system for home health-care workers, with automatic screening, structured interview support and recruitment document management. The business point is that caregiver hiring, PSW recruitment, onboarding, scheduling, training and care delivery have to work as one system.
Canada’s caregiver labour market is already tight
Canada is not short of demand for care. It is short of the workers and operating capacity needed to deliver it consistently. The federal outlook for home support workers and caregivers is not merely “competitive”; it is structurally tight. For agency owners, the implication is blunt: recruitment will stay hard, so the agencies that win must waste fewer applicants after they apply.
Table 1: Canada’s caregiver labour market is already tight
| Labour-market indicator for home support workers and caregivers | Public figure |
|---|---|
| Employment in 2023 | 67,400 |
| Workers aged 50 or older in 2023 | 49% |
| Projected job openings, 2024–2033 | 26,200 |
| Projected job seekers, 2024–2033 | 24,600 |
| Federal shortage-risk outlook | Strong risk of shortage |
Source: Government of Canada, Canadian Occupational Projection System and Job Bank.
Ontario’s aging population raises the staffing bar
Ontario shows the same pressure in sharper form. A Home Care Ontario release on McMaster research said Ontario would need 6,800 additional home-care PSWs by 2028 just to maintain current service levels. The underlying report also estimated that by the end of 2029 Ontario would have about 350,000 more people aged 75 and over.
This is why the usual advice—post more jobs, improve ads, ask for referrals—feels inadequate. It treats the labour market as if the only problem is reach. For a growing agency, the harder problem is throughput. Can the agency move the right applicants from interest to first shift quickly, safely and consistently?
Where home-care agencies lose caregivers after they apply
Most agencies can describe their client intake funnel. Far fewer can describe their caregiver funnel with the same discipline.
That is a mistake. A caregiver funnel has clear stages: application, screening, interview, background check and document collection, credential checks, training, matching, first shift, first-week review and 30-day retention. Each stage can leak. Each leak has an operational cause.
A caregiver may disappear because the agency responded too slowly. Another may drop off because document collection was confusing. A third may finish onboarding but lose confidence after a first shift with vague instructions. A fourth may leave because schedules change at the last minute and nobody explains why.
None of these failures is fixed by a better job ad. They are fixed by process.

This is where an Applicant Tracking System (ATS) helps, but only if it is tied to the rest of the agency. Automatic screening can filter applicants faster. Structured interviews can make hiring less dependent on instinct. Document management can reduce back-and-forth. But the real value appears when those steps connect to training, scheduling, care-plan visibility and early caregiver support.
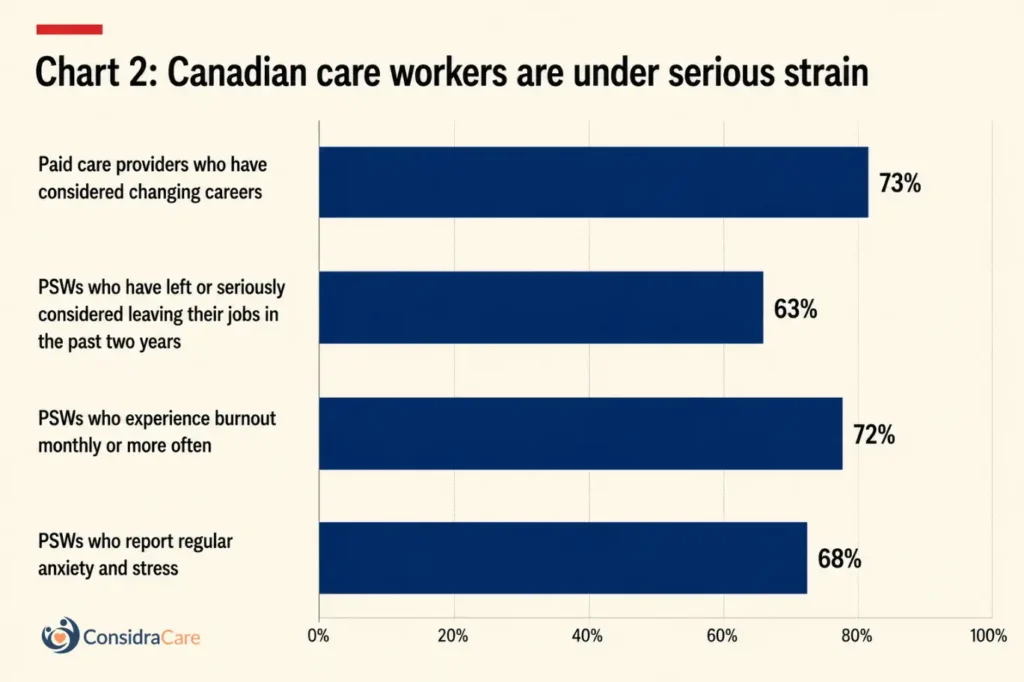
Canadian care workers are under serious strain
Agencies sometimes talk about caregiver retention as if it were only a matter of loyalty. The data suggest something harsher. Many care workers are tired, underpaid and considering leaving.
The Canadian Centre for Caregiving Excellence reported that 73% of paid care providers, including PSWs and direct support professionals, had considered changing careers, citing low compensation, inadequate staffing and lack of safety at work. A CSA Group report on personal support work found that 63% of PSWs had left or seriously considered leaving their jobs in the past two years, 72% experienced burnout monthly or more often, and 68% reported regular anxiety and stress.
An individual agency cannot fix the national wage structure or the public funding model by itself. But it can control how organized, respectful and safe its own operating environment feels. A caregiver who feels unsupported during hiring, training, scheduling or the first few shifts is already working in a market where leaving is easy to imagine.
Caregivers judge the agency before the first shift
Agencies often think of onboarding as something they do to caregivers. Caregivers experience it as evidence of what the agency is like.
A slow, confusing hiring process tells the caregiver that the agency may also be slow and confusing after the first shift. A disorganized first day suggests poor supervision. Missing documents, vague training and hurried client matching all send the same message: this place may not have its act together.
That matters because the work itself is demanding. Home-care workers deal with frailty, dementia, mobility risks, family expectations, travel time, part-time schedules and emotional labour. A caregiver who applies for overnight caregiver hiring or live-in caregiver recruitment is not just asking for hours. They are judging whether the agency can support the realities of that work.
The agency that looks organized earns trust before the first shift. The agency that looks chaotic spends the rest of the relationship trying to recover it.
Poor matching turns recruitment wins into churn
A caregiver does not stay because the hiring form was efficient. They stay because the work is manageable, the expectations are clear and the agency behaves like it knows what it is doing.
Matching is central. A caregiver who is new to dementia support should not be dropped into a complex dementia case with thin notes and no escalation path. A caregiver without a car should not be given an awkward route and then blamed for lateness. A worker who wants stable hours will not stay long if every week feels improvised.
This is where shift coverage becomes a retention issue. Owners search for “how to fill home care shifts”, “fill last-minute shifts” and “reliable caregivers for overnight shifts” because the operational pain is immediate. But last-minute coverage problems often start earlier: incomplete availability data, weak onboarding, poor matching, unclear travel expectations, missing credentials or a thin bench of workers who were never fully activated.
If the agency treats every shift gap as a scheduling problem, it will keep fighting fires. If it treats shift coverage as an onboarding and retention problem, it can start fixing the system.
Full-time employees versus contractors: the retention trade-off
Many agency owners ask whether they should hire full-time caregivers, part-time employees or independent contractors. The honest answer is that the legal, operational and retention implications are different, and the label on the agreement is not enough.
The Canada Revenue Agency says worker status depends on the facts of the working relationship. Employment and Social Development Canada lists factors such as the total relationship, control, tools, chance of profit, risk of loss and integration. Ontario also warns that misclassifying an employee as an independent contractor can lead to employment-standards consequences.
For a senior-care agency, full-time employment usually gives more control and stability. The agency can train to a common standard, assign regular clients, build culture, enforce documentation expectations and create clearer career paths. That can help retention, especially when workers want predictable income, benefits and belonging. The downside is cost and rigidity. Full-time roles require enough client volume, enough scheduling discipline and enough management capacity to keep workers productively assigned.
Contractors can look attractive because they offer flexibility. They may help cover specialized roles, short-term demand, overflow, weekend work or hard-to-fill shifts. They may also appeal to experienced workers who want more independence. But contractors are usually less embedded in the agency’s culture and may have weaker loyalty, less availability and more competing commitments. If the agency controls them like employees while calling them contractors, it also creates classification risk.
The practical answer is not ideology. Agencies should use full-time or regular employment where continuity, training, client relationships and retention matter most. They should use contractors only where the relationship is genuinely independent, carefully documented and operationally appropriate. In both cases, the agency still needs onboarding, screening, care-plan visibility, communication and documentation discipline. A bad process will lose employees and contractors alike.
Table: Full-time caregivers versus contractors
| Model | Advantages | Risks | Retention impact |
|---|---|---|---|
| Full-time or regular employees | More continuity, easier training, stronger culture, clearer supervision, better client matching | Higher fixed cost, harder to sustain without enough hours, more management responsibility | Often stronger when schedules, pay and support are reliable |
| Part-time employees | Flexible staffing pool, easier to match availability, suitable for variable demand | Fragmented schedules, weaker attachment, harder to guarantee hours | Can work well if communication and shift matching are strong |
| Independent contractors | Useful for specialized, overflow or genuinely independent work | Lower loyalty, competing commitments, less control, classification risk if managed like employees | Usually weaker unless the contractor relationship is well structured and mutually valuable |
Source note: Classification should be reviewed with legal and payroll advisers. Canadian status tests consider the substance of the relationship, not the label.
Training must prepare caregivers for real shifts
Many agencies have training. Fewer have training that changes behaviour in the field.
Operational training is different from generic orientation. It connects directly to the work a caregiver will do: reading the care plan, documenting a visit, handling family questions, escalating risks, supporting dementia clients, preventing falls, using the caregiver mobile app, respecting privacy and completing first-shift checklists.
This kind of training does not have to be elaborate. It has to be usable. A caregiver should leave onboarding knowing what the agency expects, where to find instructions, how to document care, who to contact and what to do when the visit does not match the plan.
The strongest agencies do not treat training as an isolated event. They connect it to the caregiver’s first assignments, supervisor review and early feedback. That is how onboarding becomes retention.
The first 30 days should be managed like a retention funnel
The first 30 days reveal whether the agency has hired a caregiver or merely processed an applicant.
A practical agency should know how many new hires complete their documents, finish training, accept a first shift, complete the first shift successfully and remain active after 30 days. It should know which recruitment sources produce reliable workers and which produce volume without retention. It should know whether new caregivers struggle with documentation, scheduling, client expectations or communication.
This is not bureaucracy. It is management.
A simple first-30-days dashboard might include time to first response, interview show rate, document completion time, training completion, time to first shift, first-shift issue rate, caregiver satisfaction after the first week and 30-day active status. These metrics tell the owner where the process is breaking.
Without them, the agency is left with anecdotes: “Indeed is bad,” “caregivers are unreliable,” “nobody wants to work,” or “we need more applicants.” Some of that may be true. But none of it is precise enough to manage.
The owner should not be the caregiver support system
In many mid-sized agencies, the owner is still the hidden retention system. The owner knows which caregivers are reliable, who needs encouragement, who can handle a complex client, who is upset about hours and who may leave soon.
That knowledge is useful. It is also dangerous if it lives only in the owner’s head.
A growing agency needs a system that makes caregiver support visible to the team. Applicants should move through a clear pipeline. Documents should be tracked. Interview notes should be structured. Training should be assigned and completed. First shifts should trigger check-ins. Caregiver concerns should become tasks, not memories. Supervisors should see patterns before they become resignations.
ConsidraCare’s platform is designed around that operating view. Its built-in ATS supports automatic screening, structured interviews and recruitment document management for any class of home health-care worker. The broader platform connects these hiring workflows to onboarding, scheduling, care documentation, caregiver communication and management reporting. That matters because recruitment, retention and care quality are not separate problems. They are one operating loop.
A better caregiver operating model for senior-care agencies
A stronger model has five parts.
First, the agency defines the worker profiles it actually needs: companion care, personal care, dementia support, overnight care, live-in care, nursing, therapy support or other home health roles. Hiring becomes sharper when the agency knows which roles, geographies and availability blocks matter.
Second, the agency screens automatically for minimum fit. That does not replace human judgment. It prevents the team from spending time on applicants who cannot meet basic requirements.
Third, the agency uses structured interviews. Good interviews are not scripts for politeness; they are tools for consistency. They help compare candidates fairly, test judgment and capture evidence that later informs matching.
Fourth, the agency treats document management as a speed and compliance issue. Missing police checks, credentials, work eligibility, certificates or references slow the path to first shift. In a tight labour market, delay is not neutral. Delay loses people.
Fifth, the agency links onboarding to first-shift success. The new caregiver should not be thrown into the field with a thin care plan and a phone number. They should have client context, tasks, risks, documentation expectations, directions, escalation instructions and a check-in after the shift.
That is not software for its own sake. It is an operating standard.
The economics of losing caregivers are simple
The cost of poor onboarding is often hidden because it spreads across the agency. The scheduler spends time filling gaps. The recruiter reopens roles. The owner handles complaints. The coordinator calms families. The caregiver leaves, and the agency calls the loss “turnover” rather than seeing the broken process that created it.
A simple model makes the point. Suppose an agency hires 20 caregivers in a quarter. If five drop before or shortly after the first shift, the agency has not merely lost five workers. It has lost the ad spend, screening time, interview time, document chasing, training effort and schedule planning attached to each person. It may also have lost client trust if the failed onboarding caused missed shifts or poor continuity.
The cure is not to make hiring colder or more automated. The cure is to make the routine parts systematic so managers can spend more time on judgment, coaching and relationships.
What caregiver retention means for Canadian home-care agencies
Canadian home care is a local trust business, but it now competes in a national labour reality. Workers have options. Families expect reliability. Agencies cannot afford a hiring process that depends on memory, paper files, scattered emails and heroic follow-up by the owner.
The better agency will not merely post more jobs or chase “agency staffing solutions” after every gap. It will run a tighter caregiver operating system. It will know which sources produce dependable workers, how fast applicants are screened, where documents stall, which training modules are completed, how quickly new hires reach the first shift and what happens in the first 30 days.
This is the shift: from recruitment panic to retention discipline.
Start by measuring where caregivers drop off
Do not start by buying more job ads. Start by measuring the path from application to active caregiver.
How many applicants came in last month, by source? How many passed screening? How many booked and attended interviews? How long did document collection take? How many completed training? How many accepted a first shift? How many were still active after 30 days?
Then ask the harder questions. Which applicants looked good but failed in the field? Which supervisors are best at early retention? Which clients are difficult for new caregivers? Which schedules cause the most refusals? Which training gaps show up in first-week issues?
If the agency cannot answer those questions, it does not have a recruitment problem alone. It has an operating-system problem.
Take the free agency audit or join the ConsidraCare partner pilot
If your agency is losing caregivers after they apply, interview, onboard or complete their first few shifts, start with the free ConsidraCare agency operations audit:
Take the free agency audit: https://www.considracare.com/agency-audit/
ConsidraCare is also looking for a small number of founding partner agencies to co-build better workflows for caregiver recruitment, onboarding, training, scheduling, documentation, first-shift support and management reporting.
Register interest in the partner pilot: https://www.considracare.com/book-operational-review/
The goal is not to replace human judgment in hiring. It is to stop losing good people to bad process.

- https://www.linkedin.com/in/triaz/






